People may experience cognitive changes as they age but not all changes are a normal part of aging. The changes such as memory loss may indicate the onset of dementia, so a concerned senior should go to their doctor for testing and possible referral to a specialist to ascertain the cause.
Though many older adults experience forgetfulness, serious memory loss isn’t part of the normal aging process. It could indicate dementia disorders like Alzheimer’s disease, and anyone experiencing it must consult their health care providers to know the best course of action.
How do you decide on the best doctor to diagnose and treat various kinds of dementia?
Which Are The Best Type Of Doctors Who Treat Dementia Or Memory Loss?
As we age, various changes happen within our bodies — including our brains. If you or one of your family members suffer from memory loss that doesn’t feel normal for an aging individual (e.g., asking the same question over and over, frequently becoming more confused about people and places), it’s best to talk to a doctor.
Many health care professionals can address the question. But according to the Alzheimer’s Association (ALZ), concerns like cognitive impairment are often first discussed with a primary care physician (PCP).
PCPs are trained in general internal and family medicine, allowing them to address common conditions. Skilled physicians can diagnose dementia with over 90% accuracy. When finding one, ask if they have experience identifying and managing dementia in past patients.
It’s also important to know if they know related specialists focusing on dementia. In many cases, your PCP will work with or make a referral to a specialist who is more adept at dealing with these cognitive disorders.
Is There Anything A Doctor Can Do For Dementia?
Aging is one of the biggest risk factors for dementia: Up to 8% of older adults have some form of dementia. In the US, Alzheimer’s is more prevalent among Blacks (14%), Hispanics (12%), and Non-Hispanic whites (10%).
Unfortunately, there is no cure yet for dementia disorders. If you have a loved one affected by it, know that a doctor can only help manage the symptoms and delay their progress. They’re part of a care team tasked to give patients the best quality of life possible.
One of the first things they will conduct is a thorough diagnostic process, which typically includes:
- Medical history assessment
- Review of current medications
- A physical exam
- Mental cognitive tests
- Laboratory tests (including a blood test and analysis of protein in cerebrospinal fluid)
- Psychiatry evaluations (e.g., screening for depression)
- Brain scans and imaging (e.g., magnetic resonance imaging and computerized tomography scan)
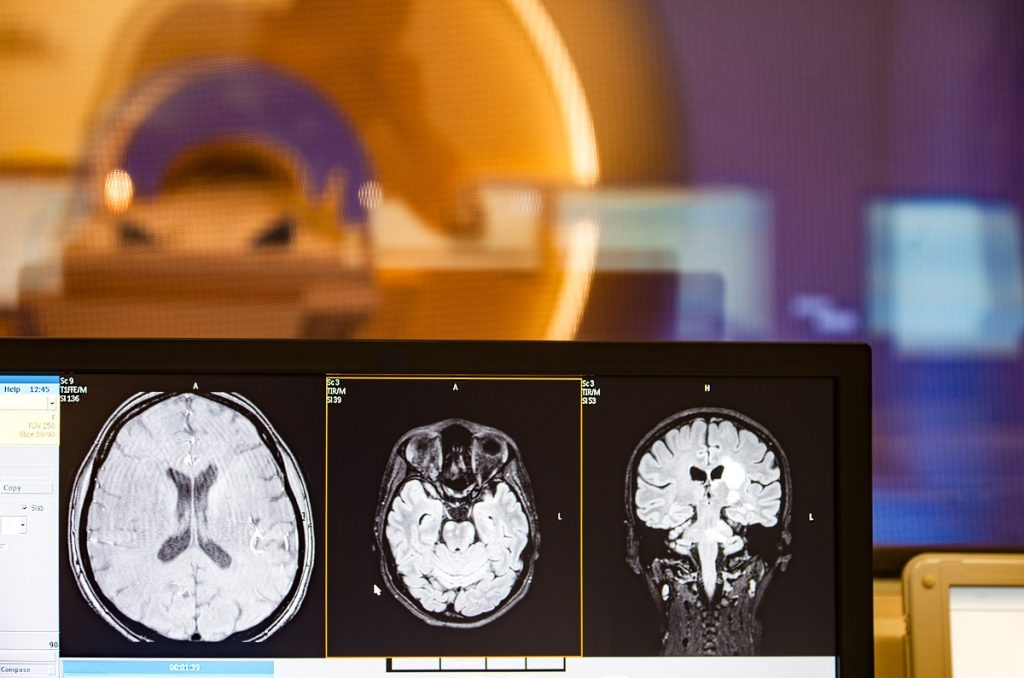
Your doctor will also recommend resources and support groups like ALZ, where you can get assistance and accurate educational materials about the condition.
Do You Need A Neurologist Or Other Specialist For Dementia?
Dementia is challenging to diagnose as most patients present unclear symptoms. This situation calls for more evaluations by at least two more specialists.
Geriatricians
Some PCPs obtain additional training for conditions and diseases that are more common among people aged 65 years and above. These PCPs are referred to as geriatricians. Seniors consult these people intending to optimize their health conditions as they age.
Geriatric Psychiatrists
These psychiatrists have received additional training in diagnosing, preventing, and treating mental disorders involving the elderly. Their experience and training help other specialists rule out other possible causes of memory issues, such as depression.
Neurologists
Focusing on nervous system disorders, neurologists (along with psychiatrists) must earn certification from the American Board of Psychiatry and Neurology.
Though not all, some of these specialists receive formal training to identify and manage different types of dementia properly. Others focus on other neurological conditions like Parkinson’s disease.

Neuropsychologists
Neuropsychologists are trained professionals who assess thinking abilities (e.g., memory, attention, problem-solving, and language). They work hand in hand with PCPs and other specialists in determining if one’s memory problems are indeed caused by dementia or other conditions that masquerade it.
What Else Might Case Dementia-Like Symptoms?
Not every memory disorder is attributable to dementia. Some medical conditions can also negatively impact how the brain works, causing patients to show dementia-like symptoms.
These conditions are usually treatable; once addressed, the cognitive impairments that come with them also get reversed. These include:
- Sleep disorders
- Hormonal imbalances
- Vitamin deficiencies (e.g., Vitamin B12, Vitamin B9)
- Dehydration
- Thyroid problems
- Low or high blood pressure
- Urinary tract infections
- Respiratory infections (including COVID-19)
- Head injury or head trauma
- Normal pressure hydrocephalus
- Medication side effects
- Mental health issues (e.g., depression, delirium)
How Do You Treat Dementia?
No medication can treat dementia itself. But PCPs and specialists can design a treatment plan to slow down its progression. It may involve the following:
Taking Medications
Acetylcholinesterase inhibitors are designed to hinder the breakdown of acetylcholine, which aid nerve cell communications in the brain. For people who cannot tolerate these inhibitors, doctors prescribe memantine.
Additional medicines may be recommended, depending if the patient has other conditions, such as cardiovascular issues and diabetes.
Receiving Person-Centered Care
Dementia-affected individuals experience a severe cognitive decline to the point that it affects their daily life. They may not be able to perform activities of daily living on their own and may be more prone to accidents and wandering.
Caregivers are there to support and help implement custom care plans either in the patient’s residence or in facilities like memory care and assisted living communities. They also help facilitate social activities and reminiscence work.
Undergoing Therapies
Dementia patients may also undergo therapies and rehabilitative programs courtesy of specialists who help address a particular concern. These may include:
- Physical therapy (to help with mobility issues)
- Occupational therapy (to teach coping behaviors and how to make their immediate environments safer)
- Counseling and cognitive behavioral therapy (to address mental health concerns)

What Are Some Warning Signs A Person Should Watch For?
How do you know if you should be diagnosed — and possibly treated — for dementia? The National Institute on Aging (NIA) enumerates these symptoms of dementia that you should be alarmed with:
- Memory loss affecting day-to-day life
- Making poor judgments and decisions
- Challenges with making plans
- Difficulty in doing familiar tasks
- Getting confused with time, place, and people
- Trouble having and following a conversation
- Misplacing things often
- Withdrawal from social activities and losing interest in hobbies
- Personality and behavioral changes
What Is The Difference Between Alzheimer’s And Dementia?
Alzheimer’s disease is just one of the many types of dementia, and it’s caused by an unusual build-up of proteins in brain cells. It’s the most common among other dementias, accounting for 60 to 80% of all dementia cases.
Dementia is a broad medical term that covers brain disorders marked by cognitive decline. Apart from Alzheimer’s, other conditions in this category are vascular dementia, frontotemporal dementia, and Lewy Body dementia.
How Does The Treatment Differ?
The treatment depends on the type/s of dementia that a patient has (in some cases, someone could have mixed dementia).
For instance, if someone has Alzheimer’s disease, their treatment plan will include taking medications that control cognitive symptoms (e.g., cholinesterase inhibitors). For vascular dementia — which occurs after a stroke has caused brain changes — there are no approved drugs yet though clinical trials showed that Alzheimer’s medicines could modestly benefit people with this type of dementia.
For frontotemporal subtypes, no specific treatment is available yet. What professionals do, however, is to reduce behavioral symptoms caused by the chemical changes affecting the frontal and temporal lobes of the patient’s brain.

